Your new post is loading...
 Your new post is loading...
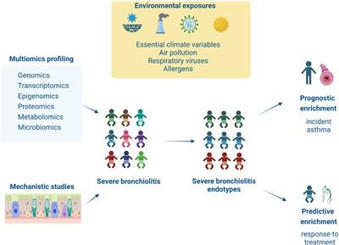
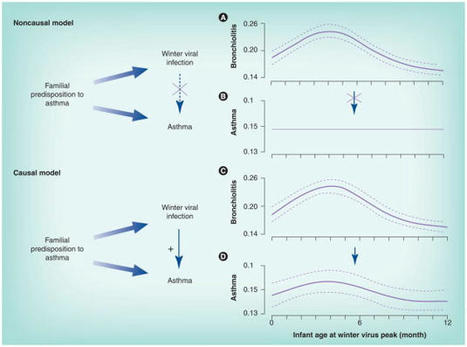
Severe bronchiolitis (i.e., bronchiolitis or first episode of wheeze requiring hospitalization) during infancy is a heterogeneous condition associated with an increased risk for childhood asthma development (1,2). Bronchiolitis cohort studies have identified early-life environmental, genetic and immune risk factors for childhood asthma development by carrying out analysis at single level (e.g., associations with respiratory virus types, host immune response or the microbiome composition of the host) (3,4). However, severe bronchiolitis pathogenesis involves interaction of factors at multiple levels (e.g., genome, epigenome, transcriptome, metabolome, microbiome). Optimistically, the increasing use of omics methodologies in observational studies allows for a more holistic approach, that can shed light on severe bronchiolitis pathophysiology by identifying distinct biological processes associated with long-term sequelae like asthma (5). In addition, mechanistic studies are required to validate and test identified pathogenetic pathways from omics studies.To further address the issues outlined above, our Research Topic congregates evidence from observational and interventional studies exploring the severe bronchiolitis to childhood asthma causal pathway with the aim to identify severe bronchiolitis endotypes that can guide predictive (i.e., response to treatment) and prognostic (i.e., association with long-term respiratory sequelae) enrichment strategies (see Figure 1). Th
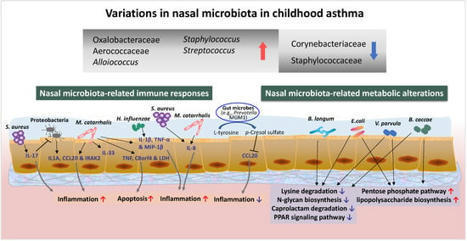
Childhood asthma is a major chronic non-communicable disease in infants and children, often triggered by respiratory tract infections. The nasal cavity is a reservoir for a broad variety of commensal microbes and potential pathogens associated with respiratory illnesses including asthma.
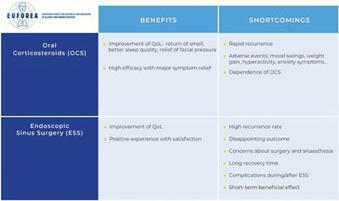
Background: European patients with chronic rhinosinusitis with nasal polyps (CRSwNP) have had only limited occasions to unite to have their voices heard, hence missing the opportunity to contribute to the improvement of CRSwNP care.Aims: To identify unmet needs in CRSwNP from the perspective of CRSwNP patients from the Patient Advisory Board (PAB) of the European Forum for Research and Education in Allergy and Airways diseases (EUFOREA).Methodology: Semi-structured interviews were conducted individually with 15 European patients with CRSwNP and with a disease history of more than 2 years. Patients shared their burden of the disease and frustrations related to CRSwNP care, experiences with key pillars of current treatment options, shortcomings of the current care pathways and recommendations for improvement of care. A panel of 30 members of the Patient Advisory Board reviewed the interview report and provided further input during 2 virtual meetings.Results: CRSwNP patients indicated the need for greater awareness from society and physicians of the disease burden with impact on social function and well-being. Along with a loss of ability to smell and the continuous presence of secretions in the nose, most patients reported poor sleep quality and psychological impact as the most bothersome symptoms. Patients' frustrations relate primarily to the underestimation of the disease burden, the lack of coordination of care and the limited treatment options available to them
Une application pensée et conçue par 5 allergologues, gratuite, pour patienter de manière ludique et fun pendant son traitement de désensibilisation, grâce à un avatar évolutif et des jeux avec scores en réseau.
We would like to bring to your attention our collection of articles in the category “Basic and Translational Allergy Immunology”, published sinc
The clinical and pathologic diagnosis of hypersensitivity pneumonitis has been confounded by conflicting definitions, with two recent guidelines suggesting that hypersensitivity pneumonitis simply be diagnosed as nonfibrotic or fibrotic.
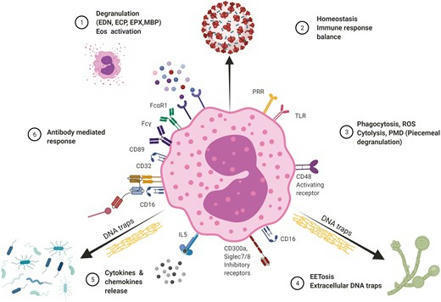
This review summarizes some of the updated information/recent findings on the role of eosinophil direct and antibody mediated interactions with pathogens.
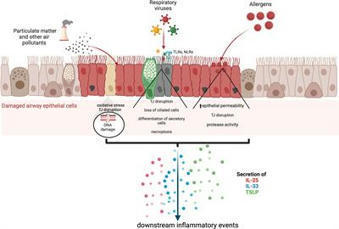
The exposure of the airway epithelium to external stimuli such as allergens, microbes, and air pollution triggers the release of the alarmin cytokines IL-25, IL-33 and thymic stromal lymphopoietin (TSLP). IL-25, IL-33 and TSLP interact with their ligands, IL-17RA, IL1RL1 and TSLPR respectively, expressed by hematopoietic and non-hematopoietic cells including dendritic cells, ILC2 cells, endothelial cells, and fibroblasts. Alarmins play key roles in driving type 2-high, and to a lesser extent type 2-low responses, in asthma. In addition, studies in which each of these three alarmins were targeted in allergen-challenged mice showed decreased chronicity of type-2 driven disease. Consequently, ascertaining the mechanism of activity of these upstream mediators has implications for understanding the outcome of targeted therapies designed to counteract their activity and alleviate downstream type 2-high and low effector responses. Furthermore, identifying the factors which shift the balance between the elicitation of type 2-high, eosinophilic asthma and type-2 low, neutrophilic-positive/negative asthma by alarmins is essential. In support of these efforts, observations from the NAVIGATOR trial imply that targeting TSLP in patients with tezepelumab results in reduced asthma exacerbations, improved lung function and control of the disease. In this review, we will discuss the mechanisms surrounding the secretion of IL-25, IL-33, and TSLP from the airway epithelium and how thi
The spectrum of immunopathogenic mechanisms underlying cow's milk allergy (CMA) is wide. Unprocessed, fresh cow's milk, like human breast milk, contains various tolerogenic factors that are impaired by industrial processing.
A Th2 immune response is central to allergic airway inflammation, which afflicts millions worldwide. However, the mechanisms that augment GATA3 expression in an antigen-primed developing Th2 cell are not well understood.
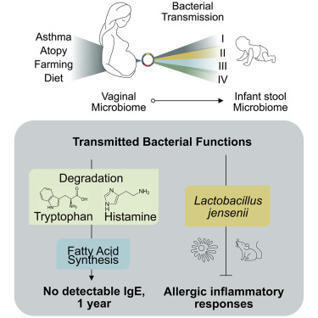
McCauley and Rackaityte et al. examine a large cohort of paired maternal-infant vaginal
and stool samples and identify shared bacteria and microbial gene functions that relate
to early-life features of atopy.
Traditional farming lifestyle has been shown to be protective against asthma and allergic diseases. The individual factors that appear to be associated with this "farm-life effect" include consumption of unpasteurized farm milk and exposure to farm animals and stables.
|
There is limited evidence on child-focused interventions that promote FAL. There is, therefore, considerable opportunity to co-design and test interventions with children.
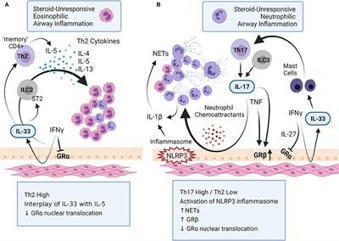
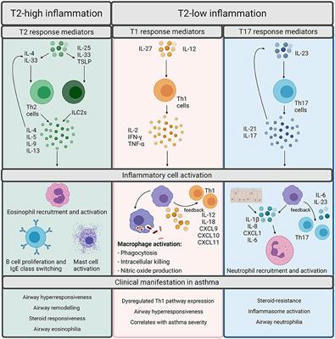
Asthma is a heterogeneous respiratory disease characterized by airflow obstruction, bronchial hyperresponsiveness and airway inflammation. Approximately 10% of asthma patients suffer from uncontrolled severe asthma (SA). A major difference between patients with SA from those with mild-to-moderate asthma is the resistance to common glucocorticoid treatments. Thus, steroid-unresponsive uncontrolled asthma is a hallmark of SA. An impediment in the development of new therapies for SA is a limited understanding of the range of immune responses and molecular networks that can contribute to the disease process. Typically SA is thought to be characterized by a Th2-low and Th17-high immunophenotype, accompanied by neutrophilic airway inflammation. However, Th2-mediated eosinophilic inflammation, as well as mixed Th1/Th17-mediated inflammation, is also described in SA. Thus, existing studies indicate that the immunophenotype of SA is diverse. This review attempts to summarize the interplay of different immune mediators and related mechanisms that are associated with airway inflammation and the immunobiology of SA.
Asthma is a heterogeneous, chronic respiratory disease affecting 300 million people and is thought to be driven by different inflammatory endotypes influenced by a myriad of genetic and environmental factors. The complexity of asthma has rendered it challenging to develop preventative and disease modifying therapies and it remains an unmet clinical need. Whilst many factors have been implicated in asthma pathogenesis and exacerbations, evidence indicates a prominent role for respiratory viruses. However, advances in culture-independent detection methods and extensive microbial profiling of the lung, have also demonstrated a role for respiratory bacteria in asthma. In particular, airway colonization by the Proteobacteria species Nontypeable Haemophilus influenzae (NTHi) and Moraxella catarrhalis (Mcat) is associated with increased risk of developing recurrent wheeze and asthma in early life, poor clinical outcomes in established adult asthma and the development of more severe inflammatory phenotypes. Furthermore, emerging evidence indicates that bacterial-viral interactions may influence exacerbation risk and disease severity, highlighting the need to consider the impact chronic airway colonization by respiratory bacteria has on influencing host responses to viral infection. In this review, we first outline the currently understood role of viral and bacterial infections in precipitating asthma exacerbations and discuss the underappreciated potential impact o
DPC mêlant vidéos et textes. Schémas et arbres décisionnels EBM pour organiser votre pensée devant une situation clinique de votre activité quotidienne.
Allergist Kathleen May, MD, of Augusta, GA was installed as president of the American College of Allergy, Asthma and Immunology at the ACAAI Annual Scientific M...
<span><b>Background:</b> This guideline addresses the diagnosis of hypersensitivity pneumonitis (HP).It represents a collaborative effort among the American Thoracic Society, Japanese Respiratory Society, and Asociación Latinoamericana del Tórax.<b>Methods:</b> Systematic reviews were performed for...
ALLERGOBIONET- Association d’Immuno-allergologie biologique hospitalière -
Dans le but de réunir leurs compétences dans le domaine de l’immuno-allergologie biologique, les praticiens exerçant dans un cadre hospitalier ont convenu de constituer une association déclarée, régie
par la Loi de 190
In this study, researchers identified significant practice variations in management & diagnosis of FPIAP among pediatric gastroenterologists and immunologists.
Respiratory syncytial virus (RSV) infects all children early in life, is the most common cause of infant lower respiratory tract infections, and causes disease exacerbations in children with asthma. Episodes of lower respiratory tract infection in early ...
Concerns have been raised about allergic reactions to messenger ribonucleic acid (mRNA) coronavirus...
All shrimp oral challenge test (OCT)-positive patients were positive for IgE against Der p 10.The level of anti-Der p 10 IgE >1.2 kUA/mL had the best diagnostic performance (sensitivity 100%, specificity 65%) Conclusion: Anti-Der p 10 IgE is useful for predicting shrimp allergy diagnosis and cou ...
|
 Your new post is loading...
Your new post is loading...
 Your new post is loading...
Your new post is loading...