Your new post is loading...
 Your new post is loading...
Researchers working at Duke University’s Pratt School of Engineering claim to have produced a laboratory first by having grown human muscle tissue that contracts and reacts to stimuli. Electrical pulses, biochemical signals and pharmaceuticals have all been used to produce reactions in the tissue that show it behaves in the same way that natural human muscles does. As a result, laboratory grown tissue may soon provide researchers with the ability to study diseases and assess drugs without invasive procedures on human subjects.
An international team of researchers has combined semiconductor nanorods and carbon nanotubes to create a wireless, light-sensitive, flexible film that could potentially act in the place of a damaged retina.
When they tested it with a chick retina that normally doesn’t respond to light, they found that the film absorbed light, sparking neuronal activity.
Patients with age-related macular degeneration (AMD), for example, could potentially benefit from such a device, the researchers from Tel Aviv University, the Hebrew University of Jerusalem Centers for Nanoscience and Nanotechnology, and Newcastle University say. AMD usually affects people age 60 or older who have damage to a specific part of the retina, limiting their vision.
While you can live without your spleen, it serves several important functions in the body including making antibodies and maintaining a reservoir of blood. It also works to keep the blood clean by removing old blood cells and antibody-coated pathogens.
Now, scientists from Harvard’s Wyss Institute for Biologically Inspired Engineering in Boston have developed an artificial spleen that has been shown to rapidly remove bacteria and viruses from blood. The technology could be useful in many scenarios, including protecting people who suffer from immunodeficiencies and those infected with difficult to treat pathogens like Ebola virus.
Regenerative medicine researchers at Wake Forest Baptist Medical Center in North Carolina have developed what they say is the most successful method to date to keep blood vessels in new human-sized pig kidney organs open and flowing with blood — a major challenge in the quest to build replacement kidneys in the lab.
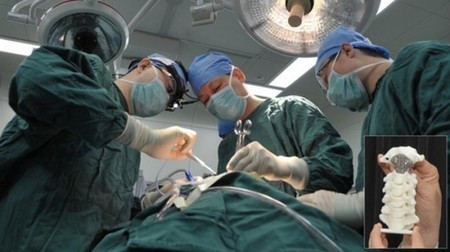
The latest surgery brought to you by the seemingly endless possibilities of 3D-printing comes at the hands of doctors at China's Peking University Third Hos...
Jeffrey Wolchok, right, works with a biomaterial that can regenerate damaged skeletal muscle (credit: University of Arkansas) A biomaterial that can
A restored functional cornea following transplantation of human ABCB5-positive limbal stem cells to limbal stem cell-deficient mice (credit: Kira Lathrop,
This February, we first heard about a bionic pancreas that could radically improve the lives of type 1 diabetics. At the time, multi-day trials involving ...
Researchers at the Fraunhofer Institute for Interfacial Engineering and Biotechnology in Germany have created a miniature artificial lung that has the potential to significantly improve the process of developing treatments for lung cancer. In addition to the possibility of replacing animal trials currently used to test new medications, the "3D-lung" could be used to expand our understanding of how lung cancer spreads to the rest of the body.
With a volume of just half a cubic centimeter, the mini-lung has is made up of human lung cancer cells growing on tissue and is attached to a bioreactor that makes it "breathe" by pumping a nutrient medium through its blood vessels. The model is therefore able to react to medication the same as real human patients.
In the field of regenerative medicine, one of the current areas of interest involves the use of scaffolding-like materials that a patient's own cells can be "seeded" onto. As the cells grow and populate the material, they gradually replace it, until all that remains is a solid piece of tissue or bone. Now, scientists at Houston's Rice University have taken that concept a step further, using a polymer that is liquid at room temperature, but that solidifies into a scaffold when injected into patients' bodies. The Rice team created a hydrogel containing a polymer known as poly(N-isopropylacrylamide), which has also recently been put forward as a "reversible glue" for temporarily sealing eye injuries while patients are in transit. As long as it's kept below body temperature, the polymer remains in a liquid state. Once heated by the body, however, it becomes a semi-solid.
If physicians have a sufficiently-early warning that a patient’s body is rejecting a transplanted organ, then there’s a good chance that they can stop the process via medication. Implanted electronic sensors could serve to provide that warning as early as possible, and thanks to new research, they’re coming a step closer to practical use.
While prosthetic limbs continue to improve, tactile feedback is one feature that many are keen to incorporate into the prosthetics but it remains a very difficult technology to develop. But now scientists have developed a new device so packed with sensors it is about as sensitive as human skin. Just as Moore’s Law continues to benefit the integrated circuit, packing ever more sensors into a smaller area will allow such devices to one day be built into everything we touch.
Some areas of our skin, like the lips and fingertips, are more sensitive to the touch because of a greater density of receptors that translate mechanical force into neuronal signals. The sensory device built by scientists at Georgia Tech is a new kind of transistor that converts mechanical force into electricity. The force bends nanoscale wires made of zinc oxide. When the wires bend back, zinc and oxide ions create an electrical potential that is converted to electrical current of a few millivolts. Converting mechanical energy to electrical energy is known as the piezoelectric effect.
Scientists have discovered yet another way to make a kidney - at least for a rat - that does everything a natural one does, researchers reported on Sunday, a step toward savings thousands of lives and making organ donations obsolete.
The latest lab-made kidney sets up a horse race in the booming field of regenerative medicine, which aims to produce replacement organs and other body parts.
|
When a medication enters the bloodstream, it ends up being concentrated in the liver – after all, one of the organ's main functions is to cleanse the blood. This means that if a drug is going to have an adverse effect on any part of the body, chances are it will be the liver. It would seem to follow, therefore, that if a pharmaceutical company wanted to test the safety of its products, it would be nice to have some miniature human livers on which to experiment – which is just what San Diego-based biotech firm Organovo is about to start selling.
Known as exVive3D, the three-dimensional liver models measure just a few millimeters across, and are created using a 3D bioprinter. The device incorporates two print heads, one of which deposits a support matrix, and the other of which precisely places human liver cells in it.
A Swedish man has recently celebrated a milestone in robotic prostheses by taking advantage of an osseointegrated (bone-anchored), thought-controlled, implant system in his daily life for more than a year and a half.
In 2009, we had a look at the Wearable Artificial Kidney (WAK) concept. The device has now been granted approval for human testing in the United States by t...
Depending on the part of the body and the nature of the injury, cartilage either doesn’t grow back at all, or does so very slowly. Now, however, researchers...
Scientists have for the first time grown a complex, fully functional organ from scratch in a living animal by transplanting cells that were originally created in a laboratory to form a replacement thymus, a vital organ of the immune system.The advance could in the future aid the development of “lab-grown” replacement organs.Researchers from the MRC Centre for Regenerative Medicine, at the University of Edinburgh, took cells called fibroblasts from a mouse embryo and converted them directly into a completely unrelated type of cell — specialized thymus cells — using a technique called “reprogramming.”
Scientists have already successfully coaxed stem cells into becoming red blood cells. Now, researchers at Brigham and Women’s Hospital have also created fun...
The ability to bio-print tissues and organs could allow us to create custom body parts that could be used for transplants. New research has brought that pos...
Artificial blood vessels are created using hydrogel constructs that combine advances in 3D bioprinting technology and biomaterials (credit: Khademhosseini
A Harvard-led team is the first to demonstrate the ability to use low-power light to trigger stem cells inside the body to regenerate tissue.
The research, reported in Science Translational Medicine and led by Wyss Institute Core Faculty member David Mooney, Ph.D., lays the foundation for a host of clinical applications in restorative dentistry and regenerative medicine more broadly, such as wound healing, bone regeneration, and more.
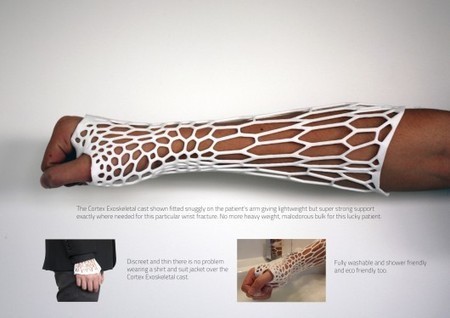
The only thing worse than breaking a bone is waiting for it to heal. During the healing process itself, wearing a fiberglass and plaster cast can be a stinky, itchy endeavor that is uncomfortable and inconvenient; all for an injury that is completely internal. Enter Jake Evill's Cortex concept. Beyond having an awesome last name, Jake Evill, a media design graduate of the Victoria University of Wellington in New Zealand, has managed to modernize the ancient concept of a splint using 3D printing technology.
MIT engineer Sangeeta Bhatia and colleagues have have identified a dozen chemical compounds that can help liver cells maintain their normal function while grown in a lab dish and also multiply to produce new tissue. Cells grown this way could help researchers develop engineered tissue to treat many of the 500 million people suffering from chronic liver diseases such as hepatitis C, according to the researchers.
Researchers at Melbourne's St Vincent's Hospital is working on developing human organs by building body cells layer by layer using a 3D printer. The team has used the 3D printer to make body cells, including muscle cells, nervous systems cells and cartilage. Professor Mark Cook, director of neurosciences at St Vincent's Hospital, said 3D body part printing was like 'bubble jet printers'.
|
 Your new post is loading...
Your new post is loading...
 Your new post is loading...
Your new post is loading...