Abstract
SARS-CoV-2 has been shown to cause wide-ranging ocular abnormalities and vision impairment in COVID-19 patients. However, there is limited understanding of SARS-CoV-2 in ocular transmission, tropism, and associated pathologies. The presence of viral RNA in corneal/conjunctival tissue and tears, along with the evidence of viral entry receptors on the ocular surface, has led to speculation that the eye may serve as a potential route of SARS-CoV-2 transmission. Here, we investigated the interaction of SARS-CoV-2 with cells lining the blood-retinal barrier (BRB) and the role of the eye in its transmission and tropism. The results from our study suggest that SARS-CoV-2 ocular exposure does not cause lung infection and moribund illness in K18-hACE2 mice despite the extended presence of viral remnants in various ocular tissues. In contrast, intranasal exposure not only resulted in SARS-CoV-2 spike (S) protein in different ocular tissues but also induces a hyperinflammatory immune response in the retina.
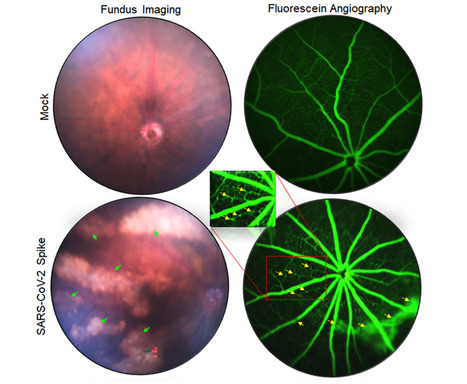
Additionally, the long-term exposure to viral S-protein caused microaneurysm, retinal pigmented epithelium (RPE) mottling, retinal atrophy, and vein occlusion in mouse eyes. Notably, cells lining the BRB, the outer barrier, RPE, and the inner barrier, retinal vascular endothelium, were highly permissive to SARS-CoV-2 replication. Unexpectedly, primary human corneal epithelial cells were comparatively resistant to SARS-CoV-2 infection. The cells lining the BRB showed induced expression of viral entry receptors and increased susceptibility towards SARS-CoV-2-induced cell death. Furthermore, hyperglycemic conditions enhanced the viral entry receptor expression, infectivity, and susceptibility of SARS-CoV-2-induced cell death in the BRB cells, confirming the reported heightened pathological manifestations in comorbid populations. Collectively, our study provides the first evidence of SARS-CoV-2 ocular tropism via cells lining the BRB and that the virus can infect the retina via systemic permeation and induce retinal inflammation.
Author summary
SARS-CoV-2 is known to cause several ocular manifestations in COVID-19 patients; however, the role of eyes in viral transmission and ocular tissue tropism remains elusive. The presence of viral remnants in various ocular tissues and fluids from COVID-19 patients has led to an assumption that SARS-CoV-2 may be transmitted through the eyes. Here, we show that SARS-CoV-2 ocular tropism is through cells lining the BRB. SARS-CoV-2 not only infects the various parts of the eye via systemic exposure but also induces a hyperinflammatory immune and antiviral response in the retina. Unexpectedly, the corneal epithelium was found to be resistant to SARS-CoV-2 infection, and ocular exposure of SARS-CoV-2 failed to cause lung pathology and moribund illness. Cells lining the BRB showed induced expression of viral entry receptors and enhanced susceptibility towards SARS-CoV-2-induced cell death, which is further potentiated with comorbidities such as hyperglycemia. Our findings from this study shed light on the role of BRB in SARS-CoV-2 ocular tropism and the role of eyes in viral transmission.
Published in PLOS Pathogen (April 10, 2024):



 Your new post is loading...
Your new post is loading...